Healthcare professionals have long recognized the association of physical activity with mortality risk—those who engage in more moderate-to-vigorous activity have lower mortality rates. In a new study, researchers across the University of Illinois Urbana-Champaign have shown that smartphones suffice to monitor people’s walking activity. They used sensor data from 100,000 participants to construct models of health status and mortality risk.
Measuring physical activity usually falls into three categories: self-reported questionnaires, walking a fixed distance under timed observation, and wearing activity monitors. The first two focus on quality of movement instead of quantity. However, sensor-based methods are the most advantageous because they measure physical activity during daily living. Unfortunately, access to such wearable sensors is limited due to health inequities.
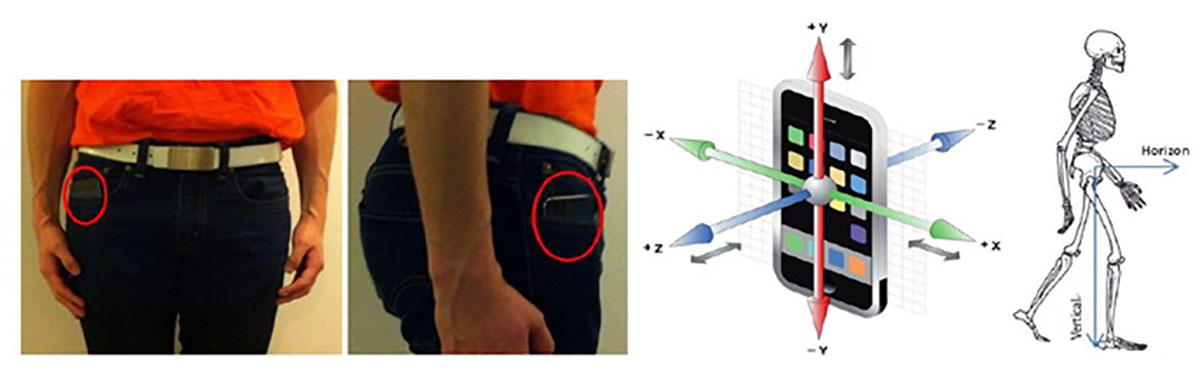
To circumvent this problem, the researchers turned to smartphones. According to the Pew Research Center, 97% of the US population own a cell phone, and 83% possess a smartphone that contains motion sensors. Since mobile phones are often carried while walking, they could be used to measure physical activity. Although the total measure of activity over 24 hours may not be possible, smartphones can be used to measure the quality of walking.
For their study, the researchers used the UK Biobank, which is the largest national cohort with sensor records that span the last 20 years. They studied 100,000 participants who were demographically representative of the UK population. The categories that were considered included age, sex, race, health disorders, previous hospitalizations, lifestyles, education levels, and income.
Each participant wore activity monitors with motion sensors for one week. Although the wrist sensor was worn differently than how an equivalent smartphone sensor is carried, the motion sensors were able to obtain information on walking intensity from short bursts of normal walking. The researchers analyzed these datasets to model the characteristic motions of these walking sessions to predict mortality risk. The UK Death Registry was used to determine which participants had passed away over a five-year timeframe.
Using Biocluster2, a high-performance computing resource at the Carl R. Woese Institute for Genomic Biology, the team was able to successfully validate predictive models of mortality risk using only 6 minutes per day of steady walking measured by the sensor. This time period is a vast improvement over the activity monitors, which assume the participants wear the sensors for 10 hours per day. The accuracy achieved was similar to physical measures such as gait speed during short walks, as well as similar to activity monitors that measure total activity.
"Our work is a big advance in health equity,” said Bruce Schatz (EIRH), a professor of library administration in the university library. “Smartphones are ubiquitous in high-income countries and increasingly common in low-income countries. Showing that they can predict mortality as accurately as existing methods implies that health monitors at a population scale are now feasible.”
There are limitations to the study that the researchers would like to address in their future studies. Although they chose a demographically representative population, low-income lifestyles differ from high-income lifestyles even when age and sex are the same. Consequently, walking tests may differ since the 6 minutes of steady walking was chosen to mimic walk tests for hospital patients with cardiopulmonary disorders. The researchers will also broaden their population samples to include the US Precision Medicine Initiative, where the participants will be representative of the US national population, which is more diverse than that of the UK. Since the models rely only on machine learning from sensor inputs, other types of health status may also be accurately predictable, such as cardiac health or asymptomatic detection of infectious diseases like COVID-19.
The research team consisted of Schatz; Haowen Zhou, a visiting scholar in the Schatz group at the IGB and now a graduate student in statistics at the University of Virginia; Ruoqing Zhu (CGD), an associate professor of statistics; Anita Ung, a staff physician at the McKinley Health Center. During this research, Schatz and Ung were faculty in the College of Medicine at the University of Illinois, using the IGB facility to collaborate with the Department of Statistics.
The study “Population analysis of mortality risk: Predictive models from passive monitors using motion sensors for 100,000 UK Biobank participants” was published in PLOS Digital Health and can be found at https://journals.plos.org/digitalhealth/article?id=10.1371/journal.pdig….
